OUR RESULTS
Before & AftersOUR NEWSLETTER
Offers & Updates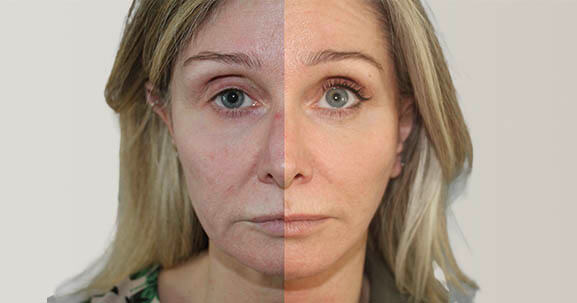


London's Leading Plastic & Cosmetic Surgery Clinic
As one of the UK’s best-known cosmetic surgeons, Alex is a leading authority in his field, trusted by new and returning clients alike. His experience and expertise mean he excels in all aspects of cosmetic surgery and he has also become renowned as the go-to gynecomastia surgeon in London. Alex and the Karidis Clinic have become synonymous with an exclusive, bespoke experience. We welcome patients from around the UK and the world, offering plastic surgery in London to help them achieve their aesthetic goals.
Our concierge team have developed the Karidis VIP Protocol to ensure your experience is seamless, from the first moment you reach out to us through to your recovery and beyond.

Our Brands